Paroxysmal nocturnal hemoglobinuria (PNH)
Disease information
Overview
Paroxysmal nocturnal hemoglobinuria (PNH) is indeed a rare and complex disease. It happens when red blood cells are missing protective proteins that normally tell the body's immune system not to attack them. Because these proteins (like CD55 and CD59) are missing or not working right, the immune system ends up destroying the red blood cells. This ongoing destruction of red blood cells can cause them to break open and release hemoglobin, which is the substance that carries oxygen in the blood.
The name "paroxysmal nocturnal hemoglobinuria" highlights a common symptom: patients sometimes have dark urine, especially in the morning, because the broken red blood cells release hemoglobin which then gets into the urine. This condition can lead to several serious health problems, including blood clots (thrombosis), kidney issues, high blood pressure in the lungs (pulmonary hypertension), damage to organs, problems with the digestive system like ischemic bowel disease, and even liver failure. It's a serious condition because it means the body's own defense system, which usually targets things like bacteria, is mistakenly attacking its own cells.

▲ The Abnormal Erythrocyte Destruction Process in Patients with Paroxysmal Nocturnal Hemoglobinuria
Causes & Symptoms
Paroxysmal nocturnal hemoglobinuria (PNH) is caused by a mutation in a gene known as PIGA, which is located on the X chromosome. However, the exact cause and mechanism of the disease have not yet been fully elucidated.
PNH is closely related to other hematologic disorders such as aplastic anemia and myelodysplastic syndromes. Notably, about 30% of patients with PNH develop aplastic anemia.
PNH has some specific symptoms such as hemolytic anemia, cytopenias, and thrombosis. However, how these symptoms show up can be very different from person to person. Some people might not show any symptoms but have lower blood cell counts, while others might have severe blood clots or kidney failure
At the beginning, you might feel tired a lot and notice that your liver or spleen has gotten bigger. The symptom we talked about earlier, where you pee dark urine at night, also known as paroxysmal nocturnal hemoglobinuria, is also a result of hemolytic anemia. When red blood cells are destroyed a lot, which we call 'hemolysis,' you might feel like you're really pale and dizzy, which are common symptoms of anemia. A lot of hemolysis can lead to a rise in harmful substances, which can cause problems like kidney failure. In situations like this, a person might be in a life-threatening condition right from when they're first diagnosed

Paroxysmal nocturnal hemoglobinuria (PNH), along with related conditions such as aplastic anemia or myelodysplastic syndrome, can lead to a decrease in red blood cells, white blood cells, and platelets. This drop in cell counts, much like in other blood disorders, can result in serious health issues, including an increased risk of infections due to the lowered number of white blood cells, and a higher chance of bleeding because of the reduced platelet count. Each patient's experience may vary, with some facing more severe complications than others.
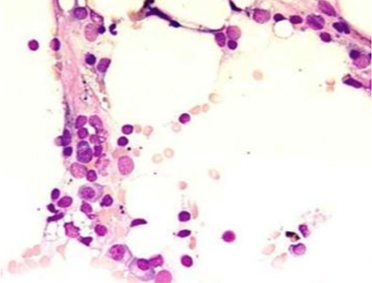
▲ In patients with paroxysmal nocturnal hemoglobinuria, it's common to see a failure of the bone marrow and related changes in the marrow
Thrombosis is the most serious complication of paroxysmal nocturnal hemoglobinuria (PNH), accounting for approximately 50% of deaths related to the condition. While deep vein thrombosis or pulmonary embolism are common sites of occurrence, thrombosis can atypically occur in various arterial or venous locations throughout the body
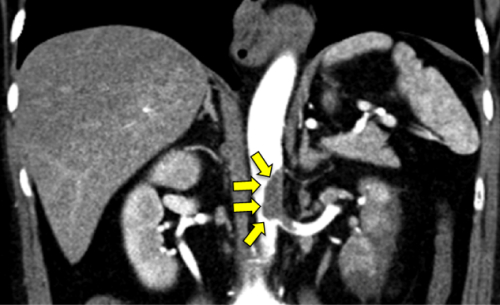
▲ Thrombosis in the abdominal aorta and renal arteries in a patient with paroxysmal nocturnal hemoglobinuria (indicated by the yellow arrows)
Treatment
Our center is dedicated to managing and treating paroxysmal nocturnal hemoglobinuria (PNH) with the goal of preventing sudden episodes and enabling our patients to enjoy a normal life. We carefully consider the specific characteristics of PNH, any associated conditions like bone marrow dysfunction, the patient's personal financial situation, and potential complications when creating an individualized treatment plan. We are committed to staying at the forefront of global advancements in targeted therapies for PNH. While these cutting-edge treatments are generally covered by insurance, the costs can still be significant. We are proud of our personalized approach to care for patients with PNH.
* Please note that the following is a basic outline of initial treatment options. We strongly advise a consultation with a physician for a detailed and personalized treatment plan.
Eculizumab, known by the brand name Soliris, is a groundbreaking treatment that specifically targets and blocks the complement system — part of the body's immune response that causes the destruction of red blood cells in paroxysmal nocturnal hemoglobinuria (PNH). By doing so, it helps prevent complications associated with PNH, including hemolysis, the process where red blood cells are broken down prematurely. Since October 2012, this medication has been covered by insurance, and its use should be discussed with a physician to see if it's right for you. Before starting Eculizumab, it's mandatory to be vaccinated against Neisseria meningitidis, a bacterium that can cause serious.
Allogeneic hematopoietic stem cell transplantation is currently the only treatment that can potentially cure paroxysmal nocturnal hemoglobinuria (PNH). However, it's a complex procedure that comes with significant risks, including complications and a risk of mortality, which must be carefully weighed during the decision-making process. The Catholic Hematology Hospital has reported a 90% long-term survival rate following transplantation for PNH, a notably high success rate in comparison to other centers. Despite these promising statistics, it's crucial for patients to discuss the potential impact on their quality of life after the transplant with their healthcare team. For those who have PNH in conjunction with bone marrow failure syndromes like aplastic anemia, stem cell transplantation might be a more actively considered option, given the nature of their condition.
Before targeted immunotherapies were introduced, steroids were the mainstay for managing chronic hemolytic anemia in conditions like paroxysmal nocturnal hemoglobinuria (PNH). Today, even with the significant symptom relief provided by targeted immunotherapies, conservative treatment with steroids remains an important option, especially for those with milder symptoms. Considering the economic aspects and the complexities involved in securing insurance coverage for newer treatments, conservative management can be a more accessible choice for some patients.
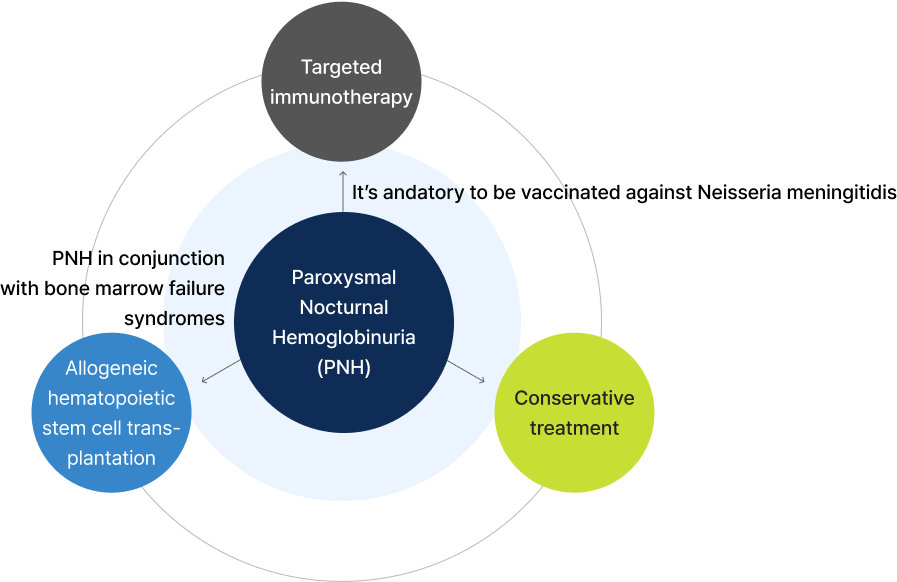
▲ Customized treatment approach for paroxysmal nocturnal hemoglobinuria

