- Home
- Disease Information
- Pediatric Hematology-Oncology Center
-
Pediatric Lymphoma
- Pediatric Acute Lymphoblastic Leukemia
- Pediatric Acute Myeloid Leukemia
- Pediatric Chronic myelogenous leukemia
- Pediatric Lymphoma
- Pediatric Aplastic Anemia
- Fanconi Anemia
- Dyskeratosis congenita (DKC)
- Pure red cell aplasia (PRCA)
- Neuroblastoma
- Osteosarcoma
- Wilms' tumor
- Pediatric Brain Tumors
- Ewing's sarcoma
- Rhabdomyosarcoma
- Hepatoblastoma
- Germ cell tumors
- Histiocytosis
Pediatric Lymphoma
Disease information
Overview
Lymphoma is a form of blood cancer that affects the lymphatic system, a crucial component of our immune defense. This system encompasses the network of lymph nodes, lymphatic vessels, lymphocytes (a type of white blood cell), as well as organs like the spleen, tonsils, thymus, and bone marrow.
Structurally akin to the circulatory system—which is made up of the heart, arteries, capillaries, and veins—the lymphatic system comprises lymph vessels and nodes through which lymph fluid circulates, carrying lymphocytes that help fight infection.
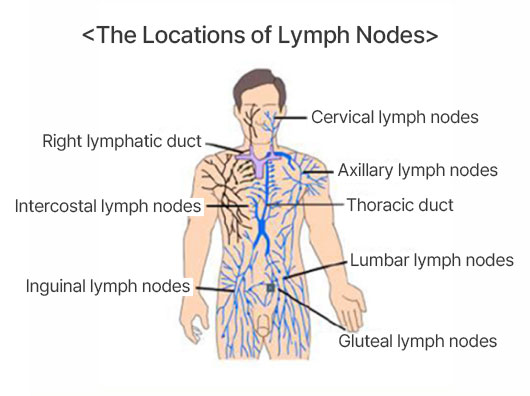
▲ Source: The Korean Society of Hematology
Lymph fluid is rich in white blood cells known as lymphocytes, and along the network of lymph vessels, there are small, bean-shaped clusters known as lymph nodes. Unique among blood cancers, lymphoma can form solid masses or tumors, similar to other solid cancers. In the pediatric population, lymphoma constitutes about 15% of all cancers, making it the third most common type of cancer in children, after leukemia and brain tumors. While lymphoma occurs in roughly 10% of childhood cancer cases, its prevalence increases significantly in adolescence, accounting for about one-third of all cancers in the 10 to 20-year-old age group.
Causes and Symptoms
The exact cause of lymphoma remains unclear, but several known risk factors have been identified. These include:
- Environmental Exposure
- Viruses
- Immunodeficiency of the immune system
Certain lymphoma types have been found to be associated with the use of immunosuppressive drugs after solid organ transplants or hematopoietic stem cell transplantation, and with infection by HIV.
A common and significant sign of lymphoma is the slow growth of a painless lump in areas where lymph nodes are located, such as the neck, armpits, and groin. While patients may not exhibit systemic symptoms at the time of diagnosis, as the disease advances, they may experience fever, night sweats, and weight loss, known as B symptoms. A significant number of patients, around 70%, show involvement of the mediastinum, the central compartment of the thoracic cavity, which can lead to symptoms like coughing if the lymphoma compresses the breathing tubes. Lymphoma can produce a variety of symptoms depending on where it's located. In its advanced stages, it can spread to the spinal canal, causing neurological symptoms, or to the central nervous system. Abdominal lymphoma might lead to fluid build-up known as ascites, changes in bowel habits, and potentially palpable masses or intestinal blockages. And if lymphoma involves the bone marrow, it may present with anemia and thrombocytopenia, conditions also common in leukemia.
Treatment
Once diagnosed with lymphoma, patients typically begin a regimen of combination chemotherapy, administered in cycles spaced 3 to 4 weeks apart. The majority of patients will notice their tumors shrink, with about 70-80% of individuals possibly achieving complete remission, meaning the tumor is no longer detectable within the body. Since lymphoma is a systemic condition, affecting the entire lymphatic system, comprehensive systemic treatment is necessary rather than just targeting the tumor location.
The type of lymphoma diagnosed, the extent of the disease, the patient’s age at onset, and the stage of the disease at diagnosis all play crucial roles in determining the chances of achieving a cure. Localized lymphoma boasts a disease-free survival rate of over 90%. For more advanced stages, such as stage 3 or 4, survival rates still remain relatively high, ranging from 60-90%. For lymphoma that returns, or recurrent lymphoma, the response to conventional chemotherapy is often less favorable. In such situations, remission is typically sought through chemotherapy first, followed by hematopoietic stem cell transplantation to try to ensure a more durable remission.
In cases where the lymphoma doesn't respond to treatment, relapses, or is recurrent or refractory and doesn't respond to conventional chemotherapy, a specific protocol is followed. If the patient responds positively to intensive chemotherapy, hematopoietic stem cells are harvested from the bone marrow and cryopreserved, or frozen and stored. After high-dose chemotherapy is administered, these stored hematopoietic stem cells are reinfused, or put back into the patient's body, to restore the function of the bone marrow. This method relies on the re-administration of the previously collected and cryopreserved hematopoietic stem cells to reestablish hematopoiesis, or the production of blood cells. This is a crucial process as it can help the body recover from the effects of the high-dose chemotherapy.
High-dose chemotherapy followed by autologous hematopoietic stem cell transplantation is a treatment used to eliminate any remaining cancer cells that can't be seen, even with a microscope. This is done by giving very high doses of chemotherapy drugs. In contrast, allogeneic hematopoietic stem cell transplantation takes advantage of the differences between the immune systems of the donor and the patient. After the transplant, the donor's immune cells can recognize and destroy the patient's remaining lymphoma cells, a phenomenon known as the graft-versus-tumor effect. However, this process can also lead to complications, the most significant being graft-versus-host disease, where the donor's immune cells may attack the patient's healthy tissues.
Immunotherapy is a relatively new form of treatment that's been making substantial progress. It works by identifying and interrupting specific signals that cancer cells display. However, these targeted therapies can't entirely replace traditional chemotherapy drugs; they often work better when used alongside existing chemotherapy treatments. Here are the targeted therapies currently being used to treat lymphoma in children.
- Rituximab (trade name MabThera) This monoclonal antibody, known as rituximab, specifically binds to the CD20 antigen present on the surface of B-cells, making it a form of targeted immunotherapy for treating B-cell lymphomas. By binding to CD20, rituximab helps direct the body's immune system to destroy the malignant B-cells.
- Brentuximab (trade name Adcetris) This treatment involves an antibody-drug conjugate engineered to target the CD30 protein, which is commonly found on the surface of Hodgkin lymphoma cells. It's employed specifically for cases where the lymphoma has either returned after standard treatments (relapsed) or has not responded to standard treatments (refractory). This approach allows for the direct delivery of chemotherapy to the cancerous cells, which can help limit the impact on healthy cells.
- Crizotinib (trade name Xalkori) This particular medication is known as a small molecule inhibitor, which is used in targeted therapy to block the action of a protein called anaplastic lymphoma kinase (ALK) found in some cases of anaplastic large cell lymphoma. By inhibiting ALK, the drug is designed to halt the progression of the disease.
- Ibrutinib (trade name Imbruvica) The medication you're referring to is engineered to specifically target and block Bruton's tyrosine kinase (BTK). BTK is an enzyme that is essential in the process by which B-cells become cancerous, and it remains active in B-cells that have turned into cancer cells. By inhibiting BTK, this drug helps to halt the growth of these cancerous cells, thereby providing a treatment option for certain types of B-cell malignancies.

